How Concerned Should We Be About COVID-19?
At this point you are likely familiar with the 2019 novel coronavirus and its disease, COVID-19. The most common questions we hear from patients are, “How serious is this, and how worried should I be?” We are also asked, “Isn’t this just like the flu?” The answers to these questions are complicated and depend on multiple factors, but there are some basic facts that can make this easier to understand.
First, I’ll address how COVID-19 compares to the seasonal flu. Regarding the risk of infection, the novel coronavirus has a higher rate of transmission. One reason for this is in the term “novel.” It is a virus that we as a population have not been exposed to and that we don’t have a vaccine to prevent. For those reasons, a higher percentage of people are expected to be infected with this virus as it spreads through our communities. Estimates of the percentage of our population that will be infected vary. A Harvard University epidemiologist, Dr. Marc Lipsitch, estimates the figure at 40 to 70 percent of the global population within the coming year(1). The other number that is frequently discussed relates to illness severity. Hospitalization rates have differed by nation, but of 44,000 cases in China, about 15 percent required hospitalization (2). At the most severe end of this is the question of how many people will die. The mortality rate has been somewhat variable in other countries but is generally considered to be at least one percent. In some locations, including Italy, the apparent mortality rate is substantially higher. Using a mortality rate of one percent, COVID-19 is ten times deadlier than the seasonal flu. So, based on how infectious it is and how deadly it can be, COVID-19 is not “just like the flu.”
Why Are the Number of Reported Cases Lower Than Those for the Seasonal Flu?
If COVID-19 is a serious disease that is expected to infect many people, why do the number of official cases and the growth of these cases still seem relatively low compared to the seasonal flu? Two major factors are at play here. One is the extremely low rate of testing. The other is exponential growth. First, there has been and, at the time of this post, remains a shortage of test kits in the United States. Thus, testing in the United States has been limited. We are just now beginning to see other testing options open, and the amount of people being tested will increase. This will lead to a significant increase in the number of official cases.
The other factor at play in the number of cases is exponential growth. Understanding this rate of growth will help you understand how a small number today can become a much larger number within just a few weeks. Experience in other countries tells us that the number of cases of COVID-19 will double approximately every six days (3). As of today, there are over 3,500 confirmed cases in the United States. Based on that figure and based on the exponential growth rate of the virus, there will be about 8,000 cases this time next week and about 18,000 the week after. Without intervention, that growth will continue until today’s small number of cases becomes far larger in just a few weeks. And, without intervention, exponential growth may not slow until millions are infected.
What Should We Do?
What should we do with this information? Don’t panic. But treat the COVID-19 pandemic as a serious matter that requires proportionally serious planning. All of us can take actions to significantly affect the outcome, making both ourselves and our fellow citizens safer. And the sooner we act, the more positive effect we can have.
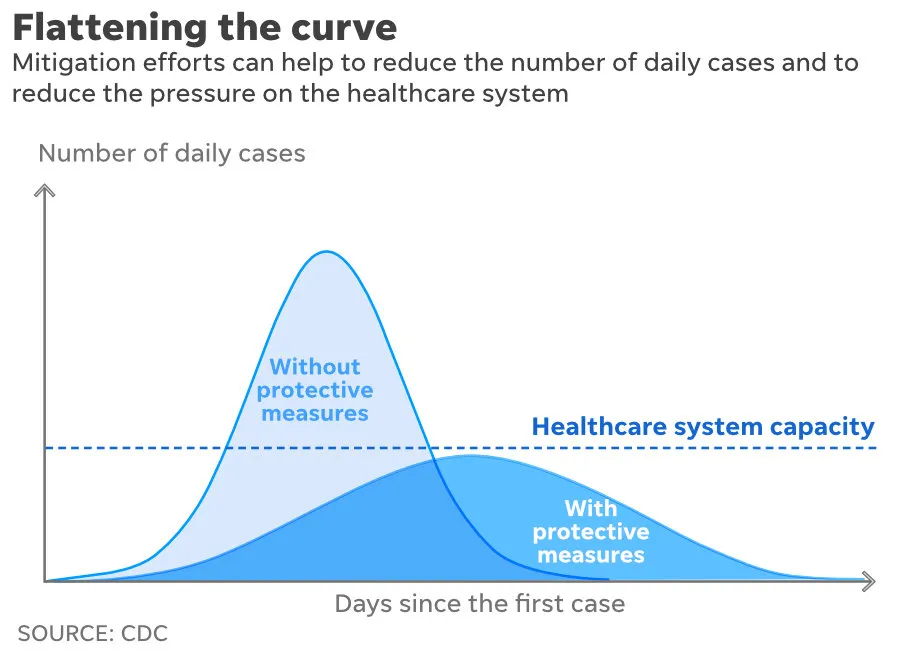
The most important action you can take as an individual is to follow the commonsense infection control procedures such as handwashing, covering your cough, and staying home if you are sick. You should immediately practice social distancing. The more we limit interaction with others, the more likely we are to slow the spread of the disease. While social distancing may not lead to lower overall infections, it can – and this is critically important – decrease the amount of people that get sick at one time. This phenomenon is generally referred to as flattening the curve. By flattening the curve, we reduce the risk of overwhelming the limited resources of our hospitals and health system. When these resources are overwhelmed, as we are seeing right now in Italy, people die who would not die otherwise. Overwhelmed resources do not only impact those who contract COVID-19. Consider that it also means if you or a loved one have a heart attack or are involved in a car wreck, hospital staff and critical care may not be readily available.
Final Thoughts
So, my recommendations to you are as follows.
- Do not panic but do treat COVID-19 as the serious matter that it is.
- Follow commonsense infection control procedures, especially frequent handwashing.
- Practice the powerful tool of social distancing to delay COVID-19’s impact.
What we and our fellow citizens do over the coming weeks will determine the extent to which COVID-19 affects all of us.
For additional information, please visit the CDC FAQ page at https://www.cdc.gov/coronavirus/2019-ncov/faq.html.
Sources
1 – https://www.theatlantic.com/health/archive/2020/02/covid-vaccine/607000/
2 – https://jamanetwork.com/journals/jama/fullarticle/2762130
3 – https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)30260-9/fulltext

Thank you Dr. Frazine for this guidance. Thankful you are our primary care doctor.
Thank you Ryan for a very clear summary of pertinent information which can inform our individual decisions and those of our church and community! Blessings to you and all colleagues and n the front lines! Pr David Deem
Excellent overview of COVID-19! And a clear explanation of what we can do to minimize overwhelming our health care resources. Thank you, Dr. Frazine!
Thank you
Thank you!
Thank you for this very needed information. Your staff has always been very helpful and understanding. All of you are in our thoughts and prayers.
Dee Beasley
Thank you doctor. More clear and honest information needs to get out . So common non medical people can understand what’s going on.
Thank you Dr. Frazine.
Thanks for reminding us about the common sense things to do. At some point it will be necessary to get out (Doctor appointments, get food, get medicine), any suggestions as the best way to handle this.
In regard to doctor visits, our office will be trying to handle as many visits as possible via telehealth video visits to minimize the need for patients to get out in public and around the hospital. Congress has voted on a measure to allow Medicare to pay for telehealth visits which they previously have not done. We have had the technology in place to do this for several months and have already performed several of these visits in the last few days.
Much has been stated on the search for a vaccine for this virus, which would benefit those not yet infected and would slow down the spread of the virus. What I haven’t heard much about is talk of remedies, or vitamins, supplements, activities (sun exposure for instance) that would mitigate the severity of the disease once contracted. As more becomes known in these areas, please comment in your blog! Thanks! I appreciate you opening this channel of communication.
Thank you. Is there a estimate time table when testing will be available in Paducah area? How and where will test be administered ??
Limited testing is available now and is being used only under strict protocols to conserve the testing for when it is most needed. We do not have any tests available in our office. Unfortunately I am not yet aware of the timeframe to expect tests to be more readily available. I expect that there will be at last one dedicated testing site up and running soon. Dedicated testing sites will allow us to minimize exposure to other patients and staff in individual offices and hopefully streamline the testing process. Patients likely will be screened via telemedicine video visit or by phone by their physician then referred for testing at a dedicated site if they meet appropriate criteria.
Thank you Dr Frazine and staff. We all appreciate your insight at these trying times. Rich Marose
What are symptoms and treatments of you have to treat yourself before testing is available? Is treatment similar as flu?
Check out this post and the linked CDC fact sheets for details on symptoms. At the current time there is no specific treatment and for mild cases the treatment is to stay at home for 14 days to avoid infecting others. In more severe cases the treatment is supportive in the hospital.